 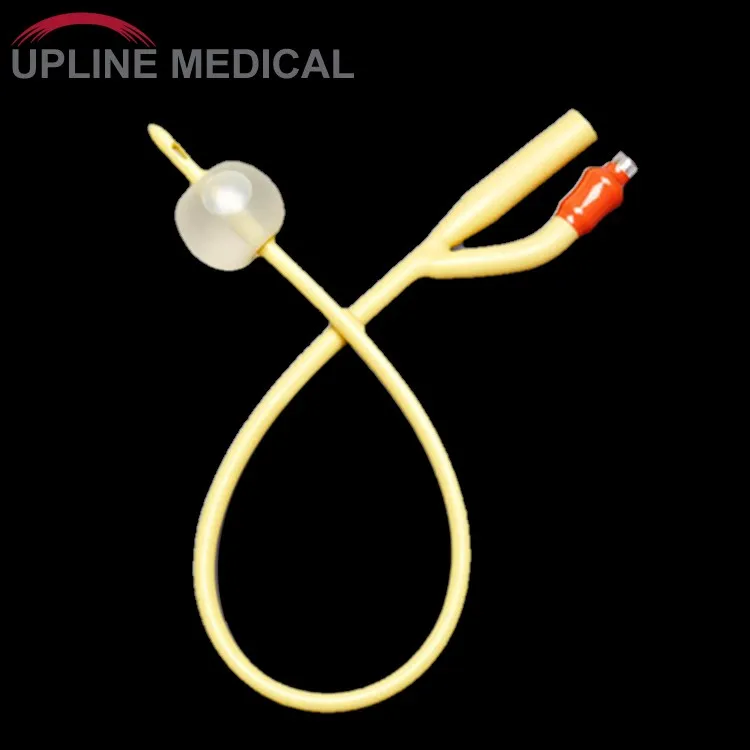
Vascularization around the gestational sac demonstrated by Doppler color flow.Īlthough there are no definitive guidelines for the management of cervical pregnancies, a variety of modalities have been proposed. Due to the acuity and urgency to stabilize the patient and to minimize bleeding, imaging to document placement could not be performed during the procedure. Once the uterine balloon was determined to be in the appropriate place, the vaginal valve was insufflated under direct visualization. Gentle traction insured that the uterine balloon of the Cook catheter was securely positioned above the internal os after insufflation. Positioning of the Cook Balloon was ascertained by visual inspection and by gentle traction. Upon insufflation, the cervix was compressed between the two balloons of the catheter and hemostasis was rapidly achieved (Figures (Figures3 3 and and4). 80 mL of normal saline was inserted in the uterine valve and 60 mL of normal saline inserted in was introduced into the vaginal valve. A silicone double balloon cervical ripening catheter (Cook Cervical Ripening Balloon) was introduced into the cervical canal (Figures (Figures1 1 and and2). After curettage, the patient continued to actively hemorrhage. Dilation and suction curettage was performed in order to excise the remaining trophoblast tissue that was readily visualized at the cervical os. After removal of vaginal packing, approximately 500 mL of additional vaginal bleeding was noted. At the time of the patient's presentation to emergency room, interventional radiology was not readily available to perform uterine artery embolization. The vaginal vault was packed with gauze in an attempt to tamponade bleeding so that patient could be safely transported to the operating room for an examination under anesthesia. On examination, approximately 300 mL of blood was cleared from the vaginal vault. The patient returned to the emergency room two days after discharge with heavy vaginal bleeding. The patient was discharged home with plan of having weekly β-hCG measured until levels declined to zero. The patient experienced no further vaginal bleeding during admission. On hospital day 7, repeat transvaginal ultrasonography showed a collapsing gestational sac with no visible yolk sac or fetal pole. Rescue leucovorin 8.5 mg (0.1 mg/kg) was administered on days 2, 4, 6, and 8. Methotrexate 85 mg (1 mg/kg) was administered on days 1, 3, 5, and 7. Uterine artery embolization was considered but concern arose about long term effects on the patient's future fertility. Decision was made to admit patient for systemic multidose methotrexate regimen for conservative management of a cervical pregnancy. 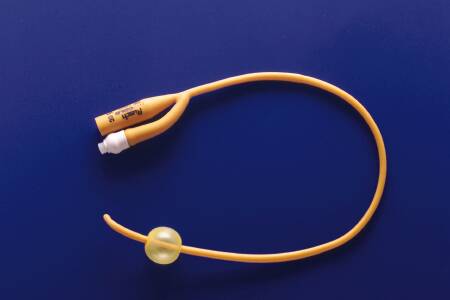
Transvaginal ultrasound revealed a 22 mm gestational sac implanted within the cervical canal with a fetal pole but no fetal cardiac activity. Her serum beta human chorionic gonadotrophin ( β-hCG) was 18,645 mIU/L. On examination, her abdomen was nontender without rebound or guarding. We describe a novel method of cervical tamponade using a silicone double balloon cervical ripening catheter (Cook® Cervical Ripening Balloon, Cook Medical, Bloomington, Indiana) in a patient that presented with acute hemorrhage after conservative management with systemic chemotherapy.Ī 31-year-old gravida 2 para 0 at 7 weeks and 3 days presented to the emergency room with complaints of vaginal bleeding and abdominal cramping that began earlier that morning. Usually more than one modality of treatment is necessary. This includes chemotherapy with methotrexate, intra-amniotic feticide, dilation and curettage, uterine tamponade, and uterine artery embolization. However, even with advanced diagnostic modalities and treatment options, CP remains a life-threatening condition.ĭuring the last decade, in an effort to avoid hysterectomy and maintain fertility, a more conservative therapeutic approach has been advocated. Early detection has been improved by ultrasonography. This type of ectopic pregnancy is highly dangerous because massive hemorrhage can ensue secondary to bleeding from the cervical vessels. Risk factors include endometrial damage after curettage or chronic endometritis, leiomyoma, intrauterine devices, and in vitro fertilization. CP accounts for less than 1% of all ectopic pregnancies. Cervical pregnancy (CP) is a rare type of ectopic pregnancy characterized by implantation of a fertilized ovum in the endocervical canal. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
